 
A, anterior P, posterior R, right L, left.DEAR DR. The patient clinically improved during that time, with resolution of both the personality changes and spells. (Bottom Panel) Brain FDG-PET 1 year after initiation of lamotrigine showed extensive resolution of the previously visualized hypometabolism. (Top Panel) Brain FDG-PET prior to initiation of antiepileptic therapy showed hypometabolism (indicated by regions in green and yellow) most marked in the left medial frontal, anterior cingulate, and medial temporal regions. (B) This 71-year-old man presented for evaluation of longstanding personality changes (starting at age 57) and more recent recurrent spells of amnesia and confusion, and displayed normal brain MRI and left frontal and right frontotemporal epileptiform abnormalities on EEG during sleep. (A) This 75-year-old man was evaluated for 6 months of amnestic spells, irritability, and disinhibition, and displayed subtle focal hypometabolism in the anteroinferior aspect of the left temporal lobe (magenta arrow) as compared to the right (teal arrow). Representative images are displayed for two individuals meeting diagnostic criteria for TEA who displayed focal hypometabolism on FDG-PET. Montage of abnormal brain FDG-PET scans in a case series of transient epileptic amnesia. FDG-PET may also complement MRI in distinguishing TEA from neurodegenerative disease when suspected.Īmnestic spells dementia memory impairment neurodegenerative disease sleep electroencephalogram (EEG). In the appropriate clinical context, our findings support the use of early prolonged EEG with emphasis on sleep monitoring as a key diagnostic tool. This syndrome is frequently associated with persistent interictal cognitive/behavioral symptoms and thus can be mistaken for common mimics. Conclusions: TEA is a treatable cause of amnestic spells in older adults. Anti-seizure therapy, most often with a single agent, resulted in improvement (reduction in spell frequency and/or subjective improvement in interictal cognitive/behavioral complaints) in all 17 cases with available follow-up. FDG-PET identified focal hypometabolism in 2/8 cases where it was performed, both involving the frontal and/or temporal regions. Brain MRI revealed focal abnormalities in only 4/19 cases (21%). In numerous cases, sleep and prolonged EEG evaluations identified abnormalities not previously seen on shorter or awake-state studies. 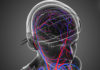
EEG revealed epileptiform abnormalities involving the frontal and/or temporal regions in 12/19 individuals (63%), including activation during sleep in all of these cases. Thirteen patients (68%) reported persistent cognitive/behavioral symptoms, including 4 (21%) for whom these were the chief presenting complaints. 
Results: Nineteen patients were identified (14 men, 5 women) with median onset age 66 years and median time to diagnosis 2 years. Diagnostic criteria included the presence of recurrent episodes of transient amnesia with preservation of other cognitive functions and evidence for epilepsy. Methods: We performed a retrospective analysis of patients diagnosed with TEA at the Mayo Clinic Minnesota from Januto September 21, 2017. Objective: To characterize the clinical, EEG, and neuroimaging profiles of transient epileptic amnesia (TEA). 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
